Frozen Shoulder Treatment aka Adhesive Capsulitis
Having trouble raising your arm out to your side above shoulder level? Has fastening clothing behind your back become nearly impossible? Whether or not you have achy/dull pain with these movements, you may have a condition called frozen shoulder. It most commonly affects women in their 40’s, 50’s, and 60’s, and is most often experienced in the non-dominant side. Frozen shoulder treatment requires an accurate diagnosis. It generally develops in three stages:
Freezing: pain gradually increases, range of motion decreases, duration 6 weeks -9 months.
Frozen: not much pain, but motion severely limited, duration 4 months -6 months.
Thawing: pain diminishes, motion is restored, duration 6 months – 2 years.
The cause of frozen shoulder is often unknown, but some predisposing factors include diabetes, autoimmune or inflammatory diseases, or immobilization. (Even wearing a shoulder sling for several weeks following a hand or wrist surgery to keep that area elevated can cause problems in the shoulder due to lack of movement).
If you’ve been to your primary care provider, they probably prescribed rest, ibuprofen, and physical therapy (PT) to strengthen and stretch your shoulder. You may have even discussed surgery if your condition has been ongoing.
The purpose of this article is to inform you of non-surgical treatment options for frozen shoulder.
While PT is generally helpful for getting stronger and more flexible, frozen shoulder doesn’t stem from weak or inflexible shoulder muscles. Another name for frozen shoulder is adhesive capsulitis, which is a fancy way of saying adhesions in the capsule of the shoulder. To further break this down, the shoulder capsule is a wrap of strong connective tissue that surrounds the bones (humerus, scapula, and clavicle) that make up the ball & socket joint of the shoulder. Adhesions (developed due to repetitive motion, lack of oxygen, or trauma) are sticky areas in muscle fibers or in the capsule itself, which limit movement, alter your biomechanics, and cause pain and dysfunction.
Strengthening a muscle does not reduce adhesion!
Stretching a muscle does not reduce adhesion!
The only way to reduce adhesion is to physical manipulate the tissues by hand or with instrument-assisted soft tissue mobilization (IASTM). Traditional treatments for frozen shoulder are Manipulation Under Anesthesia (in which the shoulder is forced to move and adhesions are broken), and shoulder arthroscopy (in which pencil-sized instruments cut through tight portions of the joint capsule to break adhesions).
New and improved frozen shoulder treatment (non-surgical):
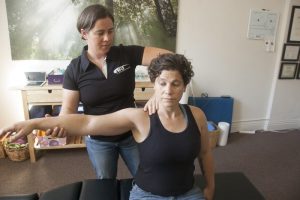
Dr. Sandy Baird utilizes Active Release Techniques (ART) protocols to reduce adhesions in the shoulder capsule. ART is the gold-standard in soft tissue treatment, and consists of several specific protocols for treating adhesive capsulitis. The treatment is gentle and precise, using hands-on manipulation of the soft tissue of the shoulder to break adhesions. A treatment for frozen shoulder will typically also require addressing adhesion in several surrounding arm and shoulder muscles, which can be performed during the same session.
Since the shoulder fails to move properly due to those deep capsule adhesions, the deltoids and some of the rotator cuff muscles spasm to try to protect the shoulder. When a muscle goes into continuous spasm, it stops receiving adequate blood flow, and the resulting hypoxia (lack of blood flow) causes adhesions to develop.
Without treatment, frozen shoulder may spontaneously resolve within one to two years. With ART treatment, most patients start to regain some shoulder motion within several visits. Frozen shoulder is one of the most difficult pathologies to treat, so patience throughout the course of the treatment plan is of the essence.
Once shoulder motion is restored and capsule adhesion is reduced, your chiropractor may introduce specific rehabilitation exercises in order to maintain your new range of motion.
If you are experiencing symptoms of frozen shoulder and would like to schedule a free consultation with an Oakland chiropractor, please call Riverstone Chiropractic at (510) 465-2342 or book your free consultation below.
Other Conditions We Treat
What Other People Just Like You Are Saying About Riverstone Chiropractic In Oakland...